HIV and AIDS
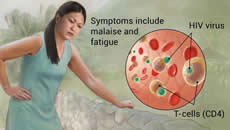 | HIV/AIDs, also called human immunodeficiency virus or acquired immunodeficiency syndrome. HIV causes AIDs and interferes with the body’s ability to fight infections. The virus can be transmitted through contact with infected blood, semen or vaginal fluids |
What is it?
- Infection with HIV causes chronic immune deficiency which, if untreated, leads to acquired immunodeficiency syndrome (AIDS) after a variable period but on average 10 years after infection. Frequently asymptomatic.
- HIV infection is treated by combination antiretroviral therapy (ART) which is life-long.
- Current evidence suggests that all people living with HIV should start ART as soon as possible after diagnosis.
- All patients need regular monitoring visits to assess their immune status, to check on response to therapy and to provide psycho-social support.
Signs and Symptoms
- Acute infection: (in 70% of patients) fever, rash, lymphadenopathy, pharyngitis, myalgia, diarrhoea, about 2 weeks after exposure
- Asymptomatic infection: for several years following infection
- Immune deficiency: multiple symptoms related to declining CD4 T-cell count such as oral thrush, diarrhoea, weight loss, skin infections, herpes zoster
Diagnosis
You can get tested for HIV by having a blood test with your GP. There is no home testing available in Australia. An early diagnosis can help you get the best treatment, prevent the progression to AIDS and reduce the chance of spreading the infection to others.
The test can take up to 24 days (and sometimes longer) following exposure for blood to show positive for infection with HIV. This is known as the ‘window’ period’. So you may need more than one test over time to know for sure if you do or do not have an HIV infection. It is important to use safe sex and safe injecting practices while waiting for the test results, and maintaining these practices after testing even if you get a negative result, will reduce your risk of future exposure and infection.
Treatment
There is no vaccine or cure for HIV infection. However, there are effective treatments such as antiretroviral medications available that can help prevent the progression to AIDS and help ensure a near-normal life expectancy.
Patients will need considerable advice and support regarding the long-term nature of therapy and the importance of good adherence. Australia does not have antiretroviral guidelines but ASHM has maintained a commentary on the US DHHS Guidelines, on which this chapter is based, except where stated otherwise. See the Antiretroviral Guidelines for more information.
Recommended follow-up
- Within a few days to check on psychosocial well-being and to review baseline investigation
- Patient will need long-term regular reviews by practitioner experienced in HIV care, via specialist clinic, sexual health service or section 100 GP
- Patient should also see GP for ongoing general care
- Once stable on antiretroviral therapy follow-up can be every 3-6 months
Contact tracing
- Notifiable condition
- Start with recent sexual or needle-sharing partners; outer limit is onset of risk behaviour or last known negative HIV test result if known
- If you have been exposed to HIV: there are medications which can sometimes prevent HIV from infecting a person who has been exposed. This is known as Post-exposure prophylaxis (PEP) can be offered within 72 hours of potential HIV exposure. See the National HIV PEP Guidelines and Policy for more information
- Pre-exposure prophylaxis (PrEP) is an important new prevention option and can provide highly effective biomedical prevention of HIV in HIV-negative individuals. See the National PrEP Guidelines for more information
For more information
- Health Direct - HIV Infection and AIDS
- Australian STI Management Guidelines - HIV Infection and AIDS
- Contact Tracing: You can now contact trace via SMS, email or send a letter to “Let Them Know” anonymously.
- Queensland Positive People: Inclusive, Innovative HIV Services
- Queensland AIDs Council
- End HIV: Prevent, Test, Treat
- Post-exposure Prophylaxis - HIV or call 13 43 25 84